All too common and requiring more than just rest
Stress fractures are one of the most common sporting injuries yet they’re often misdiagnosed in the critical early stages.
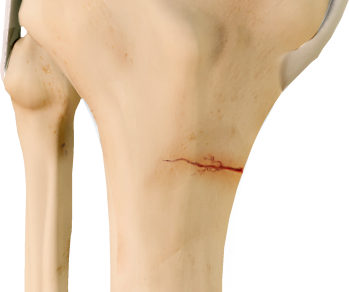
What to look out for
The most reliable feature to find on clinical examination is direct bony tenderness: even if the suspicion is low, tenderness to firm palpation over a metatarsal is a stress fracture until proven otherwise.
Even those guidelines are not foolproof. Neck of femur (hip) and pars interarticularis (spine) stress fractures can produce vaguely located pain and no localised tenderness.
Not all stress fractures behave in the typical matter but pain that is always in the same, well localised spot and increases with increased weight-bearing activity is common. If you also have localised tenderness to touch over a bony area, the suspicion is higher still.
But plenty of stress fractures still won’t be so obvious. Personally, I find that the pattern of the pain is the most reliable feature in the history: ie pain that gets worse the longer that you run that is present on impact.
A very common mistake athletes make in self-diagnosing is made in the following statement: “I couldn’t possibly have a stress fracture, I have only been training at low volumes/intensity”. Training volume is just one of the many potential contributing factors and many athletes and non-athletes develop stress fractures seemingly innocuously with very low activity levels at times.
Not all stress fractures are created equal
There are certainly grades of severity with stress injuries. Technically speaking, stress fractures that are picked up early and have stress/weakening/bruising in the bone without an actual crack going through it, are actually a stress response or stress reaction rather than a true ‘stress fracture’. The absence of a crack improves the prognosis and reduces the likely time to recovery whereas as a fracture line, a high level of bone ‘bruising’ or any amount of displacement significantly worsens prognosis and the heeling time.
This is also why it is so important to get the correct diagnosis as early as possible.
Then there are differences in different bones and locations. Metatarsals (in the foot), the fibula and the back of the tibia (shin bone) are generally pretty forgiving bones and recover quickly without much risk of complication if managed correctly.
The navicular (in the foot), front of the shin bone, scaphoid and hamate (in the wrist), neck of femur (hip) and pars interarticularae (spine) can all be nasty due to their high rate of non-union or complication such as avascular necrosis (where part of the bone dies due to a disrupted blood supply).
Then there are cancellous bones. Some bones have a hard outer shell, others are made up of the same material throughout. The latter are called cancellous bones and stress fractures to these are almost always due to insufficiency which means the bone is weak due to medical/hormonal/dietary causes rather than impact/biomechanical/training volume causes. This will also greatly influence management – but more on that later.
Whether it is in a forgiving or unforgiving location, there is no doubt that the earlier the diagnosis is made and correct treatment started, the lower the risk is of complication and the shorter the recovery time will be.
More than an Xray and Rest
There is no ‘best scan’ to get for a stress fracture. The decision is made based on the type of stress injury you’re looking for, the radiation involved and the information that is relevant at the time (ie will finding bone stress influence the treatment or are we more interested in the presence/absence of a small crack?) If the wrong test is ordered in the first place, it may delay the diagnosis or lead to a waste in time and money and unnecessary radiation exposure.
However managing a stress fracture goes well beyond making the right diagnosis early and getting the right scan. To be managed correctly, the underlying causes need to be identified and addressed and these can involve wide-ranging contributing factors such as malabsorption conditions, autoimmune diseases, hormonal dysfunction, thyroid disease, biomechanical errors and countless more. Further investigation and treatment therefore should be tailored to the individuals underlying risk factors and test results. It is for these reasons that all sport and exercise related bone stress injuries should be managed by a Specialist Sport and Exercise Physician.
Management usually involves a period of off-loading and progressive re-loading of activity at the correct level, intensity and rate while correcting any biomechanical contributing factors. There is no optimal period of rest – some early low-risk injuries can settle in a few short weeks while others need to be managed much more cautiously or even require surgery. In many cases natural supplements (such as Vitamin D and Calcium) can be helpful and in some situations we use prescription medications that can strengthen bones. When an underlying metabolic cause is identified that also needs to be treated and resolved concurrently. Many other modalities are available to achieve a faster and stronger repair of the bone when used at the right time in the right situation. These include a particular type of low-intensity pulsed ultrasound (LIPUS) that can stimulate bone repair or even using the latest technology in anti-gravity treadmill running (alter-G).
My Advice
My advice with any athletic injury is, no matter who you see, insist on a plausible diagnosis/explanation for your pain rather than just a treatment plan. If you have pain with running or walking that worsens as you go then you may have a bony stress reaction which is best investigated and managed by a Specialist Sports Physician.